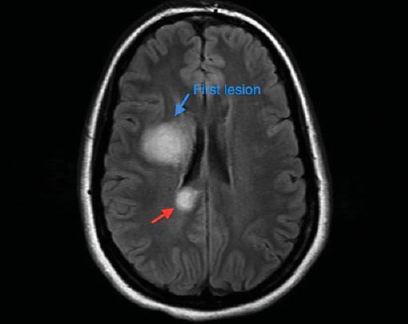
Multiple sclerosis (MS) is believed to be a neurodegenerative autoimmune disorder, in which the body’s immune system attacks its own healthy tissue, specifically the myelin sheath surrounding the axons of the central nervous system (CNS). The word sclerosis refers to the scar tissues or the plaques within brain’s white matter, observed through the Magnetic Resonance Imaging (MRI) of MS patients’ brains. These plaques are results of myelin-degeneration (demyelination) and axonal death. The progression of MS symptoms is directly proportional to the failure of remylination by oligodentrocytes, leading to neurodegeneration; this demyelination disrupts the proper conduction of action potentials from CNS to different target organs and will eventually results in permanent disability caused by chronically demyelinated plaques. Some of the common symptoms include changes in sensation, muscle weakness, abnormal muscle spasms, or difficulty moving and maintaining balance, problems in speech or swallowing, as well as visual problems.
Therefore, in addition to inhibiting the autoimmunity, preventing permanent neurodegeneration as well as functional recovery of oligodentrocytes, are current therapeutic targets in MS clinical research. The focus of this article is to discuss the several recent studies that have reported promising results to this end.
Acid-Sensing Ion Channels (ASICs) are neuronal voltage-insensitive cationic channels activated by extracellular hydrogen ions (H+), and mediate entering and excessive accumulation of sodium (Na+) and calcium ions (Ca2+) inside the neuron’s cytoplasm. This intra-axonal accrual of Na+ and Ca2+ ions causes cellular injury and subsequent neurodegeneration in the CNS. Over-expression of ASIC1 has been observed in acute MS lesions (oligodendrocytes and axons with an injury co-express ASIC1 in chronic MS lesions) and believed to play a role in the development of irreversible tissue damage.
Moreover, amiloride, a potassium sparing diuretic (causes excretion of large amounts of potassium from the body), blocks ASICs by acting as “channel-blocker” and has been used for hypertension and congestive heart failure management. In a recent translational clinical study, effects of ASIC1-inhibition was tested in 14 patients with primary progressive MS, by comparing the rates of brain atrophy and tissue damage before and during amiloride treatment for 3 years. The results of this preliminary study show a significant decrease in the rate of whole-brain atrophy during the amiloride treatment period, which indicates reduced neurodegeneration (cell damage) through ASIC blocking. Although further studies with larger populations are needed to confirm the robustness of these observations, this is a safe, inexpensive promising potential neuroprotective MS treatment that may be utilized in conjunction with anti-inflammatory agents.
As mentioned previously, failure of oligodendrocytes to remyelinate leads to the severe clinical impairments associated with MS, which makes myelin- regeneration a significant therapeutic goal. Even though oligodendrocyte precursor cells are present, they fail to mature and myelinate in MS brain. Some of the key factors stimulating migration, maturation and survival of myelinating oligodendrocytes are components of extracellular matrix (ECM).
The ECM component in areas with MS lesions have significant differences when compared with the healthy adult brain tissue: two of these ECM abnormalities are the increased expression of Laminin, as well as upregulation of Fibronectin molecule that is absent in the normal brain’s white matter. Therefore, it has been speculated that fibronectin expression in the injury environment may inhibit oligodendrocyte maturation, contributing to remyelination failure in MS plaques.
A recent study suggests that the MS inflammation in the CNS causes astrocytes to accumulate fibronectin, which impair remyelination within the chronic lesions. These findings offer new strategic clinical approaches to promote remyelination through inhibiting fibronectin aggregation and its clearance from the inflammatory sites within the parenchyma.
Interestingly, another group have recently demonstrated a strong remyelinating effect of testosterone mediated by its receptor. They propose promotion of remyelination in males with MS, through utilizing synthetic drug which specifically bine the brain androgen receptors, employing testosterone as remyelinating agents.
Although there is no approved method to efficiently treat MS up to date, there are increasing reports on not only the disease’s underlying mechanisms, but also promising clinical strategies that are rapidly moving to human clinical trials. To learn about the role of the Blood Brain Barrier and other 2013 findings in MS, visit http://info.sanguinebio.com/neurology.