Diagnosis of rheumatoid arthritis (RA) is based on meeting several of the criteria established by the American College of Rheumatology and the European League Against Rheumatism. One of these criteria is the presence of anti-citrullinated protein antibodies (ACPA). ACPA seropositivity is currently tested using a filaggrin-derived peptide (anti-cyclic citrullinated peptide [anti-CCP]) ELISA, although other ELISAs in development such as mutated citrullinated vimentin (MCV) show promising results.

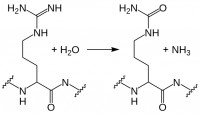
While myelin basic protein, filaggrin, and several histone proteins are naturally citrullinated, other proteins such as fibrin and vimentin can become citrullinated during an inflammatory response. Citrullination, enzymatic conversion of arginine residues into citrulline, increases protein hydrophobicity, which can change its structure. In RA, these citrullinated proteins are recognized as “non-self” by immune cells, leading to production of ACPA. Recent studies suggest these autoantibodies are not merely convenient diagnostic markers resulting from the autoimmune response, but instead may play a role in RA pathogenesis. Current research in this area includes identifying subtypes of RA based on ACPA positivity and specificity, and determining the roles and mechanisms of action for ACPA in RA autoimmunity.
Little is known about the B cells which produce these ACPA. However, in a recent report in Annals of Rheumatic Disease, Kerkman and her colleagues used B cells isolated from the peripheral blood of ACPA-positive and -negative RA patients, as well as healthy individuals, to examine ACPA production in vitro and identify the ACPA-producing cell populations.
Initially, the authors stimulated peripheral B cells with B cell activating factor (BAFF) and anti-IgM F(ab′)2-fragments to induce ACPA production. Although total IgG production was equivalent across the cultures, only B cells from ACPA-positive RA patients produced ACPA. There was good correlation of ACPA titers obtained from in vitro culture with in vivo patient ACPA titers, underscoring the utility of this model system. Next, the authors examined spontaneous ACPA production in unstimulated peripheral blood mononuclear cells (PBMC) from ACPA-positive RA patients. In this case, total IgG was up to 100x lower than that seen in their studies with stimulated B cells; however, the amount of ACPA produced was equivalent.
Were ACPA in PBMC cultures generated solely by circulating plasmablasts, or were antigen presenting cells (APC) present in the PBMC population also stimulating production of ACPA by memory or even naïve B cells? Kerkman et al. used FACS to selectively deplete ACPA-positive RA patient PBMC of plasmablast/plasma cell or naïve/memory populations, as well as to sort the CD19+ B cell subpopulations. Naïve B cells (CD20+CD27-) did not produce any ACPA, even when stimulated with BAFF and IgM F(ab′)2. Memory B cells (CD20+CD27+) produced ACPA upon stimulation, indicating CCP-specific memory cells are present in the circulation of ACPA-positive RA patients; however, ACPA production in CD20-depleted PBMC remained essentially unchanged, while unstimulated PBMCs depleted of plasmablasts/plasma cells produced significantly less ACPA.
This study demonstrates the presence of circulating ACPA-producing plasmablasts/plasma cells in the peripheral blood of patients with ACPA-positive RA. This is a novel and unexpected finding, since the plasmablast population is typically a transient population within PBMCs following antigen exposure, with antibody production continuing from mature plasma cells in the spleen and lymph nodes.
Circulating ACPA-producing B cells may persist in RA due to plasmablast replication and/or to memory B cell activation in response to persistent systemic citrullinated antigens. Currently approved RA therapies which target the CD20+ B cell population, such as rituximab, would affect the memory B cell population, but not CD20- plasmablasts. New therapies targeting circulating plasmablasts/plasma cells in addition to memory B cells could significantly limit ACPA production and subsequent immunological damage in RA, including that due to ACPA-induced TNFα production and complement activation. Delineating circulating plasmablasts as a major source of ACPA is therefore a step forward in the quest to determine the roles and mechanisms of action for ACPA in RA pathogenesis, and underscores the possibility of developing effective new therapies by targeting specific B cell populations in RA.
Further Reading:
Circulating plasmablasts/plasma cells as a source of anti-citrullinated protein antibodies in patients with rheumatoid arthritis. Kerkman PF, Rombouts Y, van der Voort EIH, Trouw LA, Huizinga TWJ, Toes REM, Scherer HU. Ann Rheum Dis 2013 Jul; 72:1259–1263.
The effect of targeted rheumatoid arthritis therapies on anti-citrullinated protein autoantibody levels and B cell responses. Modi S, Soejima M, Levesque MC. Clin Exp Immunol 2013 Jul; 173(1):8-17.
B effector cells in rheumatoid arthritis and experimental arthritis. Finnegan A, Ashaye S, Hamel KM. Autoimmunity 2012 Aug; 45(5):353-63.