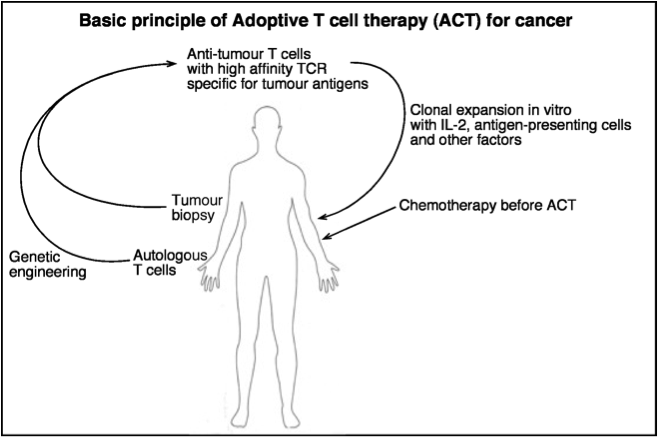
Transplantation of antigen-specific T cells during cancer immunotherapy has generated many notable results in the fight against diverse cancers. In these scenarios, the transplanted T cell populations act as a sort of highly mobile army that can track and kill tumor cells wherever they hide. In contrast, the goal of therapy during autoimmunity is to suppress immune activity, not increase its potency. Would transplantation of a “peacekeeper” immune cell-type be able to specifically quell autoimmune reactions? T regulatory cells (Tregs) are attractive candidates for the peacekeeper role based on their ability to dominantly suppress auto-reactive cell populations. As opposed to studies of cancer immunotherapy, clinical trials for Treg adoptive transplant are hampered by the lack of specific cell surface markers for these populations that enable their purification1. The defining characteristics of Treg populations (eg. FoxP3, IL-10, TGF-beta) are intracellular proteins whose analysis and quantification requires permeabilization and, hence, destruction of the cells. Positive selection for markers such as CD4 and CD25 which are expressed on the surface of certain types of Tregs also enriches for effector T cell populations whose functions upon transplantation may serve to further stimulate immune activity in an autoreactive host.
In this month’s issue of Nature Medicine, Gagliani et al. sought to address the need for Treg-specific cell surface markers2. The authors focused on a particular type of inducible Treg called Type 1 regulatory T cells (Tr1 cells). These are a highly suppressive population of CD4+ T cells that are thought to control immune reactions both through IL-10 secretion and direct, Granzyme B-mediated destruction of myeloid antigen presenting cells. Galiani et al. were able to isolate Tr1 clones from the peripheral blood of healthy donors using a limiting-dilution assay: CD4+ T cells were plated in wells at a density of 1 cell/well, grown in conditions known to be suitable for Tr1 development, and then assessed for high levels of IL-10 secretion. The isolated Tr1 clones were stimulated in vitro and their gene expression profiles were measured at different time points and compared to that of naïve CD4+ T cells (Th0 cells). Under these conditions, the authors found that Tr1 cells uniquely expressed genes for two cell surface markers, CD49b and LAG-3. Used independently, these markers would enrich for multiple T cell types. But when used in combination, CD49b and LAG-3 allowed the investigators to isolate Tr1 cells from human peripheral blood which expressed high-levels of IL-10 and were able to suppress T cell proliferation in vitro. The authors went on to show that this cell-surface marker combination could also be used to isolate Tr1 cells from well-defined mouse models of Treg function. Finally, authors showed that CD49b and LAG-3 could effectively enrich for Tr1 cells from a highly-expanded, in vitro-polarized bulk population. This raises the possibility of generating large numbers of highly pure IL-10 secreting Tr1 cells for adoptive transplantation during autoimmunity.
Gagliani et al. have effectively used gene profiling of a target cell type to identify cell-surface markers for a previously difficult-to-analyze population. These new markers should facilitate further clinical study of adoptive transplant of Treg populations for autoimmunity. Now that it is possible to identify Tr1 cells from blood, it will be interesting to see how numbers of these cells correlate to different disease states and how they change in response to immune modulatory treatments. Furthermore, coupling the polarization and enrichment of Tr1 cells to tetramer-based identification of antigen-specific T cells may allow for highly-selective targeting of autoimmune reactions.
References:
1. Human T regulatory cell therapy: take a billion or so and call me in the morning. Riley JL, June CH, Blazar BR. Immunity. 2009 May;30(5):656-65. doi: 10.1016/j.immuni.2009.04.006.
2. Coexpression of CD49b and LAG-3 identifies human and mouse T regulatory type 1 cells. Gagliani N, Magnani CF, Huber S, Gianolini ME, Pala M, Licona-Limon P, Guo B, Herbert DR, Bulfone A, Trentini F, Di Serio C, Bacchetta R, Andreani M, Brockmann L, Gregori S, Flavell RA, Roncarolo MG. Nat Med. 2013 Jun;19(6):739-46. doi: 10.1038/nm.3179. Epub 2013 Apr 28.