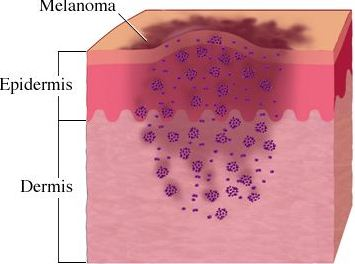
Melanoma is a type of skin cancer that arises from specialized pigmented cells in our body known as melanocytes, which are responsible for the production of melanin (a pigment responsible for skin and hair color). Because most melanoma cells still make melanin, melanoma tumors are usually brown or black. It accounts for 4% of all skin cancers; however, it is responsible for the largest number of skin cancer related deaths in the world. In the U.S, according to the national cancer institute, estimated new cases and deaths from melanoma in 2013 will be 76,690 and 9,480 respectively (for details please refer to my blog titled “targeting B-RAF kinase in melanoma”).
B–RAF is a serine/threonine protein kinase that activates the mitogen activated protein kinase (MAPK) signaling pathway. Approximately 50% of melanomas harbor activating BRAF mutations among which mutations at codon 600, resulting in substitution of glutamic acid for valine (B-RAFV600E), are the most prevalent. Activated BRAF phosphorylates and activates mitogen-activated protein kinase kinase proteins (MEK1 and MEK2), which then activate downstream MAP kinases. The MAPK pathway is implicated in the regulation of proliferation and survival of tumor cells in many cancers. This suggests that both B-RAF and its downstream MEK kinase could serve as attractive targets in cancer therapeutics. In 2011, the U.S. Food and Drug Administration (FDA) approved vemurafenib for the treatment of V600E B-RAF mutated melanoma patients. As a single agent, vemurafenib resulted in some degree of tumor regression among 90% of melanoma patients early in the course of treatment. Continuing with the effort to target B-RAF and MEK, several studies tested the efficacy of other compounds to inhibit these components of the MAPK pathway. Based on international clincal trials, on May 29th, 2013, the U.S FDA approved two new drugs Tafinlar (dabrafenib) and Mekinist (trametinib) for use in advanced melanomas with B-RAF V600E mutation. Mekinist is also approved for another form of B-RAF mutilated patients, V600K, which accounts for approximately 10% of B-RAF mutated metastatic melanoma. The mutation status of the melanoma patients are detected by an FDA-approved test, such as companion diagnostic assay from bioMerieus S.A., and THxID-B-RAF.
Tafinlar (dabrafenib) is an orally bioavailable B-RAF-inhibitor which selectively binds to and inhibits the activity of mutated B-RAF (V600E). The FDA approval of dabrafenib is based on an open label multicenter phase III study where 250 were randomly assigned to receive either dabrafenib (187 patients) or dacarbazine (63 patients). Dacarbazine is an alkylating agent which is also use to treat malignant melanoma. The study observed a statistically significant increase in progression-free survival (PFS) in patients treated with dabrafenib, compared to dacarbazine. With dabrafenib, the median PFS was 5.1 months and overall response rate was 52%. The most common adverse reactions with dabrafenib were skin-related toxic effects, fever, fatigue, arthralgia, and headache.
Trametinib is an orally bioavailable inhibitor of MEK which specifically binds to and inhibits MEK 1 and 2, resulting in an inhibition of growth factor-mediated cell signaling and cellular proliferation in various cancers. The FDA approval of trametinib is based on the phase 3 open-label trials which randomly assigned 322 patients who had metastatic melanoma with a V600E or V600K BRAF mutation to receive either trametinib or dacarbazine or paclitaxel (a mitotic inhibitor used in cancer chemotherapy). The study observed a statistically significant increase in PFS in trametinib treated patients compared to other treatments. The PFS was 4.8 month for patients treated with trametinib, while with other chemotherapeutic treatments it was 1.5 months. Rash, diarrhea, and peripheral edema were the most common toxic effects noted following trametinib treatment.
GlaxoSmithKline, manufacturer of both new drugs, reported that the products would be available no later than the early part of the third quarter of 2013.