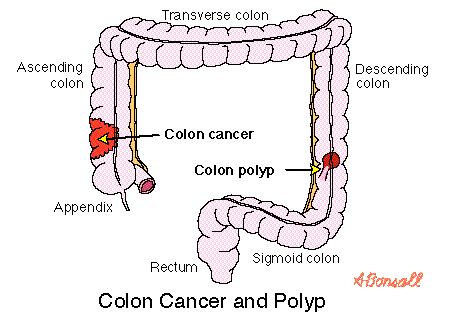
Colorectal cancer (CRC) originates in the tissues of the colon (the longest part of the large intestine), rectum and appendix, and is also known as colon cancer. Most CRCs are adenocarcinomas (cancers that begin in cells that make and release mucus and other fluids). According to the National Cancer Institute (NCI) the estimated new cases of colorectal cancer in the United States in 2013 will be 102,480.
Based on the genetics and etiology of the disease, CRC is usually classified into three specific types: sporadic, inherited, or familial.
Sporadic colorectal carcinomas:  Account for approximately 70% of CRC. Sporadic carcinomas are devoid of any familial or inherited predisposition and are common in persons over 50 years of age.
Account for approximately 70% of CRC. Sporadic carcinomas are devoid of any familial or inherited predisposition and are common in persons over 50 years of age.
Inherited colorectal carcinomas: This group of CRC includes those in which colonic polyps (an extra piece of tissue that grow in the colon) are a major manifestation of disease and those in which they are not. The nonpolyposis predominant syndromes include hereditary nonpolyposis CRC (HNPCC) (Lynch syndrome I) and the cancer family syndrome (Lynch syndrome II).
Familial colorectal carcinomas: This is the least understood pattern of CRC. In affected families, CRC develops too frequently to be considered sporadic but not in a pattern consistent with an inherited syndrome. Up to 25% of all cases of CRC may fall into this category.
Several studies suggested that like many other types of cancers accumulation of genetic changes were also associated with the development of CRC. Each of these event confers selective growth advantage, ultimately results in uninhibited cell growth, proliferation, and clonal tumor development. Two major mechanisms of genomic alterations that have been implicated in CRC development and progression are chromosomal instability and microsatellite instability. In addition, genes which have been implicated in the tumorigenesis of CRC include p53, p16, p14, APC, β-catenin, E-cadherin, Transforming Growth Factor (TGF)–β, SMADs, MLH1, MSH2, MSH6, PMS2, AXIN, STK11, PTEN, DCC, and KRAS. Among these, oncogenic mutation of KRAS is considered a standard molecular biomarker that predicts the clinical benefit for targeted inhibition with epidermal growth factor receptor (EGFR) inhibitors. The EGFR-targeted monoclonal antibodies cetuximab and panitumumab are effective only in a subset of metastatic CRC, and 50% patients who initially respond to cetuximab or panitumumab develop resistance through KRAS mutations. Emergence of secondary resistance to anti-EGFR antibodies has also been implicated through expression of EGFR ligands, HER2 amplification, and deregulation of EGFR recycling process. Altogether, these account for 70-80% of the cases of resistance to anti-EGFR antibodies. This suggests that there might be additional mechanisms of resistance to these agents in CRC.
A recent study by Bardelli et al. (Cancer Discovery, June 6, 2013), the authors addressed the molecular basis of resistance to anti-EGFR therapy in CRC patients who did not develop KRAS mutations. In their study, Bardelli and colleagues identified amplification of the MET proto-oncogene responsible for acquired resistance. Presence of the MET amplicon was detected 3 months after therapy initiation in circulating cell-free DNA of CRC patients. The role of MET amplification in limiting the efficacy of anti-EGFR antibodies was further verified in preclinical CRC models and in patient-derived colorectal cancer xenografts. Marked tumor regression was observed in these models when tumors were treated with a MET inhibitor JNJ-38877605 combined with cetuximab. Therefore, collectively this study suggests that a CRC patient population developing resistance through MET amplification could benefit from combined treatment of MET inhibitor with anti-EGFR monoclonal antibody.
REFERENCES:
Bardelli A, Corso S, Bertotti A, Hobor S, Valtorta E, Siravegna G, Sartore-Bianchi A, Scala E, Cassingena A, Zecchin D, Apicella M, Migliardi G, Galimi F, Lauricella C, Zanon C, Perera T, Veronese S, Corti G, Amatu A, Gambacorta M, Diaz LA, Jr., Sausen M, Velculescu VE, Comoglio P, Trusolino L, Di Nicolantonio F, Giordano S, Siena S (2013) Amplification of the MET Receptor Drives Resistance to Anti-EGFR Therapies in Colorectal Cancer. Cancer Discov 3: 658-673.
Center MM, Jemal A, Smith RA, Ward E (2009) Worldwide variations in colorectal cancer. CA Cancer J Clin 59: 366-378.
Misale S, Yaeger R, Hobor S, Scala E, Janakiraman M, Liska D, Valtorta E, Schiavo R, Buscarino M, Siravegna G, Bencardino K, Cercek A, Chen CT, Veronese S, Zanon C, Sartore-Bianchi A, Gambacorta M, Gallicchio M, Vakiani E, Boscaro V, Medico E, Weiser M, Siena S, Di Nicolantonio F, Solit D, Bardelli A (2012) Emergence of KRAS mutations and acquired resistance to anti-EGFR therapy in colorectal cancer. Nature 486: 532-536.
Sameer AS (2013) Colorectal cancer: molecular mutations and polymorphisms. Front Oncol 3: 114.